Reduced gestational weight gain with lifestyle intervention
1. Women receiving dietary counseling and exercise classes had less gestational weight gain than those receiving standard prenatal care.
2. There were no differences in gestational diabetes, operative delivery or birth weight between intervention arms.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Excessive gestational weight gain has been associated with adverse maternal and neonatal outcomes including postpartum weight retention, gestational diabetes, preeclampsia, large for gestational age (LGA) infants, and childhood obesity. Current guidelines for recommended weight gain in pregnancy are BMI-dependent such that women with low BMI <18.5 kg/m2 are recommended to gain 28-40 pounds (lbs), women with normal BMI between 18.5 and 24.9 kg/m2 are recommended to gain 25-35 lbs, overweight women with BMI between 25-29.9 kg/m2 are recommended to gain 15-25 lbs and obese women with BMI ≥30.0kg/m2 are recommended to gain just 11-20 lbs. While these guidelines have been promoted worldwide, a significant proportion of women, particularly overweight and obese women, continue gaining too much weight in pregnancy. Lifestyle interventions to counter gestational weight gain and its associated adverse pregnancy, neonatal and maternal health outcomes cons are a growing area of interest. Prior studies focusing on overweight or obese women before pregnancy suggested that exercise and diet interventions could be used to decrease gestational weight gain and the risk for gestational diabetes.
This trial evaluated the impact of an exercise and diet intervention and found that while the intervention was associated with decreased gestational weight gain, there were no effects on maternal or neonatal outcomes. Strengths of the study were single-blinded randomized controlled trial design and implementation in an existing health care system. Limitations included random 1:1 allocation such that women were not randomized by pre-pregnancy BMI and in fact more overweight women were randomized to the intervention arm, which may bias results toward the null. Only women who felt capable of performing the exercise component of the intervention were included in the study such that results may be limited by selection bias and may not apply to women who less motivated to exercise. RCTs in all women, and especially overweight and obese women, are needed to determine whether a threshold gestational weight gain exists beyond which pregnancies are at greater risk for adverse outcomes for both mother and baby.
Click to read the study in BJOG
Relevant Reading: Effects of interventions in pregnancy on maternal weight and obstetric outcomes: a meta-analysis of randomized evidence
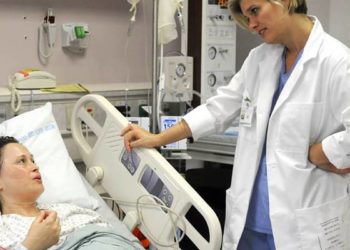
In-Depth [randomized controlled trial]: This study evaluated the impact of a lifestyle intervention consisting of dietary counseling delivered via telephone and twice weekly exercise classes on gestational weight gain and maternal and neonatal outcomes in 296 women. The control group (n = 295) in this study received routine prenatal care and an informational pamphlet about nutrition and exercise during pregnancy. The primary outcomes of interest were gestational weight gain, infant birth weight, maternal fasting glucose levels and adiposity and operative deliveries.
Women in the intervention group gained 1.3 kg overall (p = 0.009) and gained weight at a slower rate than their control arm counterparts (p = 0.03). A nonsignificantly larger proportion of women in the control arm exceeded gestational weight gain guidelines (p = 0.056). No differences in any maternal or neonatal outcomes were observed.
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.