Repeat bone mineral density testing may not improve prediction of fracture outcomes
Image: PD
1. Repeat bone mineral density (BMD) scans did not meaningfully change risk stratification for major osteoporotic or hip fractures in men and women not undergoing treatment for osteoporosis.
2. Serial BMD scans may not provide clinically meaningful information and may not justify the cost associated with the test.
Evidence Rating Level: 2 (Good)
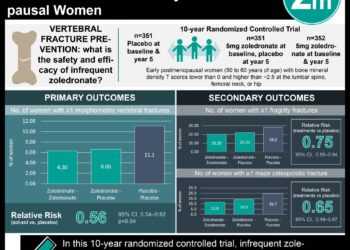
Study Rundown: Bone mineral density (BMD) scans are used to predict the probability of osteoporotic fractures and are an important component in decisions regarding treatment of osteoporosis. The utility of repeat BMD scans, however, is controversial. This study aimed to understand the role of repeat BMD scans in individuals not treated for osteoporosis. Individuals from the Framingham Osteoporosis Study who had two BMD scans were followed for 12 years after the second BMD scan or until 2009 for hip or major osteoporotic fracture. The BMD change over the average time between scans did help predict the risk of major osteoporotic or hip fractures. Therefore, follow up scans provide little information that cannot be gleaned from baseline scan results. Strengths of this study include a relatively large sample size of 802 individuals and the relatively long follow up period. This study included only individuals in an untreated population, and further research should be done to elucidate the utility of serial BMD scans in a treated patient population.
Click to read the study published today in JAMA
Relevant Reading: Rate of Bone Density Change Does Not Enhance Fracture Prediction in Routine Clinical Practice
In-Depth [prospective study]: This study included 802 individuals (310 men, 492 women) from the Framingham Osteoporosis Study. The average age at the time of the first BMD scan was 78.4 years, the average length of time between scans was 3.7 years, and the median length of follow up after the second BMD scan was 9.6 years. Women, individuals with lower BMI or BMD, and individuals with prior fractures were more likely to experience major osteoporotic or hip fractures in this study. At 10 years’ follow-up, participants with a BMD change of 1 standard deviation below the mean had a 14.1% absolute risk of hip fracture. Receiver operator characteristic (ROC) curve analysis was performed to assess the association between baseline BMD and change in BMD to major osteoporotic or hip fractures. They found that the ROC curve with the baseline BMD was slightly superior to that with BMD change (AUC 0.71, 95% CI 0.65-0.78 vs. AUC 0.68 95% CI 0.62-0.75).
By Jeffrey Cohen and Brittany Hasty
More from this author: Link of low vitamin D with coronary heart disease varies by race, Most physicians point to others to control healthcare costs, QRS morphology and duration associated with cardiac resynchronization outcomes, New genetic link between type 2 diabetes and coronary heart disease
© 2013 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.