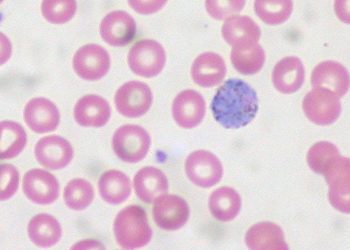
Severity of malaria infection may be independent of parasite burden
Image: PD
1. While severe malaria infections occurred during high-densitiy parasitemia, most high-density infections did not result in clinically severe malaria.
2. Prior mild or moderate infection with plasmodium falciparum did not appear to reduce the risk of severe infection or high-density parasitemia; though recurrence of severe infection was extremely rare.
3. Naturally acquired resistance to severe infection did not appear to depend on control of parasite burden.
Evidence Rating Level: 2 (Good)
Study Rundown: This study aimed to clarify the pathogenesis of severe malaria and acquired immunity by tracking parasite burdens and clinical infections in a cohort of Tanzanian children. Through periodic clinical examinations and blood testing, the authors demonstrated that high parasite burden is necessary, though not sufficient, to produce clinically severe malaria. While severe malaria infections occurred during high-density parasitemias, many high-density infections were not severe and some were asymptomatic. Additionally, most severe infections occurred after children had already had at least one infection. These findings suggest that prior exposure alone is not sufficient to protect against severe infection and also that suppression of parasite load may not be necessary. As with any cohort studies, this study was susceptible to hidden confounders and possible intervention bias. For example, the treatment of malaria may have affected development of immunity among the children. Nevertheless, this study provides convincing evidence that immunity to severe malaria is not related to control of parasite density but instead may be related to virulence of the parasite or host response. Further studies should aim to clarify these mechanisms.
Click to read the study, published today in NEJM
Relevant Reading: World Malaria Report 2013
Study Author, Dr. Patrick E. Duffy, MD, talks to 2 Minute Medicine: Chief and Senior Investigator, Laboratory of Malaria Immunology and Vaccinology Division of Intramural Research, NIAID, NIH
“Our birth cohort study has shown that most Tanzanian children suffer severe malaria after their first infection, and not at the time of their heaviest parasite burdens. Children become immune after 1 or 2 severe malaria episodes, and usually long before they are able to control parasite burden during infection. A vaccine against severe malaria should try to reproduce this type of immunity.”
In-Depth [prospective cohort]: The authors enrolled newborns in the Muheza district of Tanzania between 2002 and 2005. Researchers examined the children every 2 weeks during infancy, then monthly after infancy, as well as during any reported illness. They collected blood smears with each examination. Any p. falciparum identified on blood smear counted as a parasitemia. High density infection was defined as 2500 parasites per 200 white cells. They additionally tested samples for p.falciparum-specific histidine-rich protein 2 (PfHRP-2) levels via ELISA (thought to be a better measure of total parasite mass as parasite sequestration can skew quantification in blood smears). Clinical infection severity (severe, moderate or mild) was defined by pre-determined clinical criteria based on the WHO definition. Children were followed for an average of 2 years, but some as long as 4. 81% of children had at least 1 infection, while 11.6% had severe malaria. While mean parasite densities were significantly higher during severe infections (p<0.001) but most high-density infections did not result in severe malaria. The incidence of severe malaria, but not high-density infections, decreased after infancy. 70 of 102 (69%) of severe infections occurred after at least one prior infection. Only 3 of 102 (2.9%) of severe infections occurred in children who had already experienced one or two severe infections.
More from this author: Pneumocystis linked to sudden infant deaths, Continuous infusion of beta-lactams may be superior to bolus therapy, Novel antiviral drug reduces influenza viral load, Three months of antibiotics appear to effectively treat early-onset spinal implant infections
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.