Sigmoidoscopy reduces colon cancer risk for men, but not women
1. Sigmoidoscopy was associated with a reduction in the prevalence of colon cancer mortality in men.
2. Sigmoidoscopy did not appear to have a significant protective effect for women with respect to decreasing the rates of colorectal cancer.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Colorectal cancer (CRC) is one of the most common cancers in men and women in the United States. Current practice guidelines recommend CRC screening in adults aged 50 to 70, through colonoscopy, flexible sigmoidoscopy, or a fecal occult blood test. Although sigmoidoscopy is one of the current screening methods, its efficacy remains unclear in men and women, as further studies with longer-term follow-up are needed. Therefore, the purpose of this study was to evaluate the effectiveness of flexible sigmoidoscopy in terms of screening for CRC in men and women. Overall, the results of the study suggested that while sigmoidoscopy reduces colon cancer risk for men, this trend is not apparent in women. One of the study’s strengths is the long-term follow-up, where participants were evaluated at approximately 15 years. Limitations of the study include the fact that data on socioeconomic status and ethnicity were not available. While the study was randomized, these factors may still have had an influence on the results. Furthermore, results of this study may not be generalizable to all populations.
Click to read the study, published in Annals of Internal Medicine
Relevant Reading: Effectiveness of flexible sigmoidoscopy screening in men and women and different age groups: pooled analysis of randomised trials
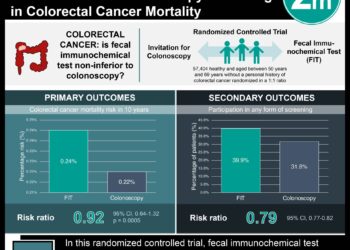
In-Depth [randomized controlled trial]: The authors of this study conducted a randomized controlled trial to evaluate the efficacy of flexible sigmoidoscopy in terms of CRC screening. The trial involved men and women aged 50 to 64 without CRC at baseline, with primary outcomes including CRC incidence and mortality stratified by sex. In general, sigmoidoscopy was associated with a reduced rate of mortality from CRC in men. For example, the absolute risk for death of CRC in men was 0.49% for the screening group, compared to 0.81% for the control group (risk difference, -0.33 percentage point [CI, -0.49 to -0.16 percentage point]; HR, 0.63 [CI, 0.47 to 0.83]). This trend was not apparent for the women involved in the study. Specifically, the treatment group for women had an absolute risk of death of 0.60%, while the control group had an absolute risk of death of 0.59%. The screening adherence rates of the study were 64.7% in women and 61.4% in men.
Image: CC/Wiki
©2018 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.

![2MM: AI Roundup- AI Cancer Test, Smarter Hospitals, Faster Drug Discovery, and Mental Health Tech [May 2nd, 2025]](https://www.2minutemedicine.com/wp-content/uploads/2025/05/Untitled-design-350x250.png)