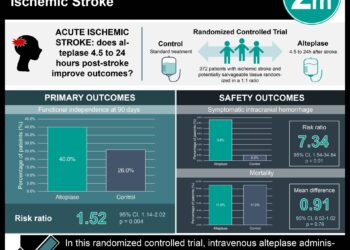
Stroke expansion following intra-arterial therapy may explain worse outcomes
1. Following complete revascularization by intra-arterial therapy, growth of the core infarct occurred in approximately one-third of patients suffering large vessel occlusive ischemic strokes.
2. Significant infarct growth and worse clinical outcomes despite therapy was associated with Hispanic race and inversely associated with pre-interventional administration of an intravenous thrombolytic and the use of stent-retriever devices.
Evidence Rating Level: 2 (Good)
Study Rundown: Due to the considerable clot burden present in large vessel occlusive strokes, systemic therapies such as intravenous (IV) thrombolysis are frequently unable to achieve complete revascularization. Because of this, there has been growing interest in the use of directed intra-arterial therapy (IAT), which was recently shown to significantly improve outcomes in patients with large vessel stroke. However, a sizable portion of IAT stroke patients nevertheless suffer poor outcomes despite complete revascularization and technological improvements in intra-arterial interventions, and the reasons for this are not fully understood. The current study sought to determine if, given successful revascularization, these patients displayed continued growth of the ischemic region as a potential explanation for such inferior clinical outcomes. Through an examination of patients with large vessel occlusion in the anterior circulation who underwent complete recanalization by IAT, the authors showed that approximately one third of patients displayed significant interval infarct growth by magnetic resonance (MR) or computed tomography (CT) perfusion imaging as compared to baseline infarct imaging. Subgroup analyses revealed that Hispanic race was associated with an increased risk of infarct growth, while pre-interventional IV thrombolytic administration and the use of stent-retriever devices were independently associated with a reduced risk of infarct growth. The study was limited by its small sample size, placing question on the significance of the racial predilection for poorer outcomes, particularly given the lack a control for stroke etiology among enrolled patients. Additionally, the heterogeneity among the imaging modalities employed and the timing of the perfusion imaging used to assess infarct core size for both baseline and follow-up creates a potential confounder. Of note, these methods were not well suited to formally address vessel patency to determine if re-occlusion occurred. A future randomized controlled trial employing a systematic examination of both core infarct size and vessel patency to compare newer IAT techniques with and without IV thrombolysis is warranted to expand on these initial findings.
Click to the read the study in Journal of NeuroInterventional Surgery
Relevant Reading: Intra-arterial prourokinase for acute ischemic stroke (PROACT II)
In-Depth [retrospective cohort]: Sixty patients were enrolled having met the baseline criteria of complete large vessel occlusion in the anterior circulation followed by complete recanalization (graded modified Thrombolysis In Cerebral Infarction 3 or 2c reperfusion) by IAT. Of those enrolled, 34 (56%) were male and mean age was 67 ± 13.7 years. Baseline perfusion imaging to determine core infarct size was performed using MR imaging in 26 (43%) of patients, while the remaining patients were examined by CT perfusion imaging. Using this, the baseline mean core infarct volume was calculated as 17.1 ± 19.1 mL. Patients then underwent IAT with subsequent re-examination of core infarct volume an average of 6.3 ± 9.5 days later. A threshold value for significant infarct growth of >11 mL was utilized based on the DEFUSE cohort trial, and this threshold was met at follow-up imaging in 35% of subjects. Subgroup analyses revealed that Hispanic race was associated with increased infarct growth (P = 0.04) while the use of pre-procedural IV thrombolysis (P = 0.03) and stent-retriever devices (P = 0.03) were inversely associated. Follow-up clinical examination at three months showed that 23% of patients with significant infarct growth had a poor outcome, indicated by a modified Rankin Scale score of £2 versus 48% of patients without significant infarct growth.
More from this author: Imaging of atherosclerotic inflammation possible with fluorine MRI, Dual-energy CT may improve detection of acute small bowel ischemia, Pancreatic cancer screening with MRI may benefit high-risk patients
Image: CC/Wiki
©2014 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. No article should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2 Minute Medicine, Inc.