The EVS: Vitrectomy results in better visual outcomes for light-perception patients [Classics Series]
1. In patients with endophthalmitis after recent lens implantation, immediate vitrectomy significantly improved visual outcomes for patients presenting with light-perception visual acuity compared to vitreous tap. In patients with better than light-perception vision at the time of presentation, there was no benefit with vitrectomy.
2. Systemic antibiotics do not provide any further benefit when added to intraocular antibiotics in either vitrectomy or vitreous tap.
Original Date of Publication: December 1995
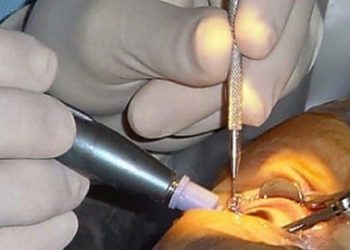
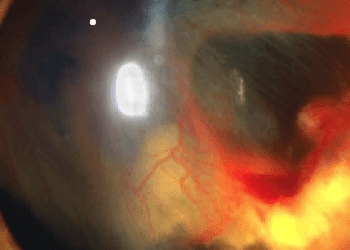
Study Rundown: Endophthalmitis is a condition characterized by inflammation of all intraocular structures, usually secondary to bacterial infection, and is one of the most challenging complications of ocular surgery. Vitrectomy, a procedure to remove vitreous humor from the eye, was thought to be advantageous in managing endophthalmitis, though prior studies were inconclusive and often suffered from selection bias. Furthermore, while intraocular antibiotic injections were considered standard of care, the role of systemic antibiotics remained unclear.
The Endophthalmitis Vitrectomy Study (EVS) was a randomized controlled trial that sought to establish the role of pars plana vitrectomy and systemic intravenous antibiotics in the treatment of endophthalmitis. The study found that, in patients with light-perception (LP) visual acuity at presentation, immediate vitrectomy tripled the frequency of achieving 20/40 vision, doubled the frequency of achieving 20/100 vision, and reduced the frequency of severe vision loss by half. In patients with better than LP visual acuity at presentation, vitrectomy was not shown to be beneficial compared to vitreous tap/biopsy. Systemic antibiotics were found to have no benefit and were not recommended as part of routine endophthalmitis treatment to reduce side effects, cost, and hospital length of stay.
Click to read the study in JAMA Ophthalmology
In-Depth [randomized controlled trial]: This multicenter, randomized controlled trial recruited patients with clinical signs and symptoms of bacterial endophthalmitis after having cataract or lens implantation in the preceding 6 weeks, with obscured second order arterioles either due to hypopyon or cloudy media (but clear enough to view the iris and perform pars plana vitrectomy), and a visual acuity between 20/50 and light-perception (LP). Exclusion criteria included pre-existing eye disease limiting best corrected visual acuity beyond 20/100, previous intraocular surgery apart from simple cataract surgery or lens implantation, and previous treatment for endophthalmitis. A total of 420 patients were randomized using a 2×2 factorial design to i) vitrectomy (VIT) or b) vitreous tap/biopsy (TAP) and i) intravenous antibiotics (amikacin and vancomycin) or ii) no intravenous antibiotics. Patients were followed for 9-12 months. The primary outcomes were visual acuity and ocular media clarity at final visit.
At 3 months, patients treated with VIT experienced higher rates of clear media than patients receiving TAP (86% vs. 75%, p = 0.004). This difference was not seen at the final study visit, except in patients with initial LP vision (VIT 78% vs. TAP 52%, p = 0.007). Comparing patients who received systemic antibiotics with those who did not, there was no significant difference in media clarity noted at any time. There were no differences between the VIT and TAP groups in terms of achieving 20/40 or 20/100 visual acuity, though VIT therapy did significantly reduce the risk of severe visual loss (5/200 or worse) compared to TAP (8% vs. 15%, p = 0.03). Again, systemic antibiotic treatment did not influence the likelihood of visual improvement. In the subgroup of patients with LP vision initially, VIT resulted in significantly greater chances of achieving 20/40 vision (33% vs. 11%) and 20/100 vision (56% vs. 30%), and a lower chance of severe visual loss (20% vs. 47%) when compared to TAP (p < 0.001 for all comparisons).
Image: PD
©2017 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.