The NLST trial: Screening for lung cancer [Classics Series]
Image: PD
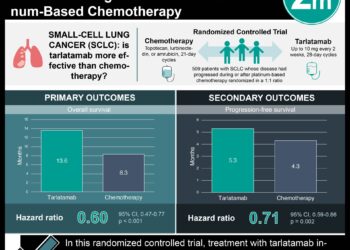
1. Low-dose computed tomography screening reduces lung cancer mortality when compared to screening with chest radiography
2. Screening for lung cancer with either modality resulted in very high false positive rates
Original Date of Publication: August 4, 2011
Study Rundown: Prior studies have shown that lung cancer screening using chest radiography does not decrease lung cancer mortality. The use of molecular markers in screening is also under study, but currently unsuitable for clinical application. In contrast, observational studies have suggested that low-dose helical computed tomography (CT) may be superior to chest radiography in detecting early-stage lung cancer. The National Lung Screening Trial (NLST) was a randomized, controlled study that compared 3 annual low-dose CTs with chest radiography in lung cancer screening. In summary, this study demonstrated that low-dose CT screening significantly reduced lung cancer-related mortality when compared with chest radiography (RRR 20.0%; 95%CI 6.8-26.7, p=0.004). Additionally, low-dose CT screening detected more lower-stage cancers than chest radiography and low-dose CT significantly decreased all-cause mortality.
Strengths of the study include the participants’ high adherence rate. Approximately 95% of participants adhered to the three rounds of screening in the low-dose CT group, while 93% adhered in the radiography group. Advancements in CT scanners since the time of the study may lead to further reductions in lung cancer mortality, though may also contribute to higher rates of false positives. The major limitations of this study are the limited follow-up and the very high false-positive rates in both the CT and radiography groups. Recently, the United States Preventive Services Task Force issued a draft statement recommending screening high-risk individuals with low-dose CT on an annual basis based on the results of the NLST trial, though there remains a lot of controversy in this area. The American Cancer Society, for example, recommends discussing screening with low-dose CT, while cautioning patients about the high likelihood of false positives and potential further investigation.
In-Depth [randomized, controlled study]: Originally published in NEJM in 2011, the NLST was a randomized trial that enrolled 53,454 patients. Eligible patients were between 55-74 years of age, had at least a 30 pack-year smoking history, and, if former smokers, had stopped smoking within the last 15 years. The exclusion criteria were a previous diagnosis of lung cancer, having a chest CT in the previous 18 months, hemoptysis, or unexplained weight loss in the previous year. In the end, 26,722 patients were randomized to screening through three annual low-dose CTs and 26,732 to three annual chest radiographs. Chest radiography, rather than community care, was chosen for the control group because the concomitant Pancreatic, Lung, Colorectal, and Ovarian (PLCO) cancer trial was evaluating the effect of chest radiography versus community care for lung cancer. Data analysis was conducted according to the intention-to-screen principle. For low-dose CT, any non-calcified nodule smaller than 4 mm in diameter was classified as a positive finding. For chest radiography, any non-calcified nodule was classified as a positive finding. Results showed that low-dose CT was associated with a significant 20.0% relative reduction in lung cancer mortality (95%CI 6.8-26.7, p=0.004). Low-dose CT was also associated with significantly higher incidence of lung cancer (RR 1.13; 95%CI 1.03-1.23). All-cause mortality was significantly lower in the low-dose CT group by 6.7% (95%CI, 1.2-1.36, p=0.02).
By Evan Chen and Andrew Cheung, M.D.
©2013 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.