The WOEST trial: Double vs. triple therapy in patients requiring PCI and anticoagulation [Classics Series]
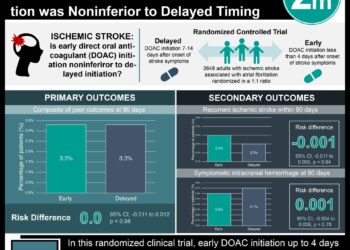
1. In patients requiring percutaneous coronary intervention (PCI) and long-term oral anticoagulation, treating with clopidogrel alone (i.e., double therapy) significantly reduced the risk of bleeding when compared to a combination of aspirin and clopidogrel (i.e., triple therapy).
2. There were no differences between the two groups in the risk of myocardial infarction, stroke, target vessel revascularization, or stent thrombosis.
Original Date of Publication: March 2013
Study Rundown: Many patients, like those with atrial fibrillation or mechanical heart valves, require long-term oral anticoagulation. A significant proportion of these patients also suffer from ischemic coronary artery disease requiring PCI, and subsequently, require dual antiplatelet therapy for a certain period of time in addition to anticoagulation. Combining these therapies, however, results in a high-risk of bleeding to the patient, with an uncertain benefit in reducing the risk of thrombosis. The purpose of the What is the Optimal antiplatelet and anticoagulation therapy in patients with oral anticoagulation and coronary StenTing (WOEST) trial sought to address these uncertainties. Patients who had an indication for long-term anticoagulation and required PCI were recruited to the trial and randomized to either antiplatelet therapy with clopidogrel alone (i.e., double therapy), or a combination of aspirin and clopidogrel (i.e., triple therapy), which was standard at the time, in addition to their anticoagulation. In summary, patients treated with double therapy had a significantly lower risk of bleeding than those on triple therapy. Moreover, there were no significant differences between the two groups in the risk of myocardial infarction, stroke, target vessel revascularization or stent thrombosis.
Click to read the study in The Lancet
In-Depth [randomized controlled trial]: This open-label, randomized trial was conducted at 15 sites in the Netherlands and Belgium. Patients were eligible for the study if they were between 18 and 80 years of age, had an indication for long-term anticoagulation (e.g., atrial fibrillation, mechanical heart valve), and had a severe coronary lesion with indication for PCI. Exclusion criteria included a history of intracranial bleeding, cardiogenic shock, a contraindication to aspirin, clopidogrel or both, thrombocytopenia with platelet count <50×109/L, major bleeding in the past 12 months, and pregnancy. Included patients were randomized to either clopidogrel alone (i.e., double therapy) or a combination of aspirin and clopidogrel (i.e., triple therapy) in addition to their anticoagulation. In the case of bare metal stents, antiplatelets were taken for 1 month and up to 1 year, while antiplatelets were administered for at least 1 year in patients with drug-eluting stents. The primary endpoint was any bleeding episode during the 1-year follow-up. The composite secondary endpoint included death, myocardial infarction, stroke, target-vessel revascularization and stent thrombosis.
A total of 573 patients underwent randomization. At 1-year, patients in the double therapy group experienced significantly lower risk of overall bleeding compared to the triple therapy group (HR 0.40, 95%CI 0.28-0.58, p < 0.0001). The rates of major bleeding, however, were no different between the two groups (HR 0.56, 95%CI 0.25-1.27, p = 0.159). Patients in the double therapy group also experienced significantly lower risk of the composite secondary endpoint (HR 0.60, 95%CI 0.38-0.94, p = 0.025), as they had significantly lower risk of death (HR 0.39, 95%CI 0.16-0.93, p = 0.027) than patients on triple therapy. There were no significant differences between the two groups in the risk of myocardial infarction, stroke, target vessel revascularization or stent thrombosis.
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.