Use of prescription drugs affecting fracture risk not changed after fracture
1. In a retrospective cohort study of Medicare beneficiaries, there was no overall change in prescribing patterns of drugs that increased or decreased fracture risk before and after fragility fractures.
2. There was a subset of patients for whom the prescribing of high risk medications decreased, but this was matched by new prescriptions of these medications for other patients.
Evidence Rating Level: 2 (Good)
Study Rundown: For an aging population, fragility fractures are common and are associated with significant morbidity and mortality. While risk of fragility fractures is affected my many non-modifiable factors such as age, gender, and genetics, decreasing the use of medications associated with fragility fractures presents an opportunity to improve care. Medications that can increase risk of fragility fractures include those associated with increased falls (sedatives, hypnotics, opioids, antihypertensives), decreased bone density (glucocorticoids, PPIs, anticonvulsants), or through unknown mechanisms (antipsychotics). Medications that help reduce the risk of fractures include bisphosphonates.
This study evaluated the use of prescription medications that increased or decreased risk of fractures to evaluate changes in prescribing patterns following incident fractures. The results showed that use of studied medications did not change significantly following fragility fractures. There was a subset of patients for whom the use of implicated medications decreased, however this was matched by new prescriptions for other patients. Additionally, there was not a clinically significant increase in the use of bisphosphonates following the fragility fracture. This study highlighted the importance for in-depth review of medications following major medical events such as fragility fractures. The weakness of the study included not evaluating the overall outcomes after the incident fracture. Also, the study did not explore the indication for the medications used.
Click to read the study, published today in JAMA Internal Medicine
Relevant Reading: Fall risk-increasing drugs and falls: a cross-sectional study among elderly patients in primary care
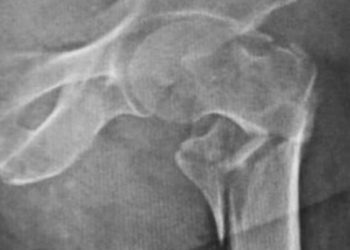
In-Depth [retrospective cohort]: This study evaluated 168 133 patients with a fragility fracture (hip, shoulder, or wrist), from 2007 to 2011. Patients were Medicare beneficiaries enrolled for at least 4 months who resided in the community (rather than skilled nursing facility), and were excluded if they were enrolled in hospice, nursing home, or did not fill any prescriptions during the study periods. A total of 21 drug classes were investigated due to prior studies linking them to increased risk of fragility fractures. These included: benzodiazepines, barbiturates, opioids, hypnotics, SSRIs, antihypertensives, diuretics, glucocorticoids, PPIs, antipsychotics and others.
Prior to the index fracture, 76% of patients were on at least one study medication in the preceding 4 months. Following the fracture, the proportion of patients on at least 1 non-opioid implicated medication was 80.5% for hip fractures, 74.3% for wrist, and 76.9% for shoulder. There was a group of patients with reduced use of medications implicated in fracture risk, but this was matched with a group of patients that began new medications with fracture risk. The use of drugs that increase bone density did rise following fragility fractures significantly (p < 0.001), however the absolute number was very small (21.1% vs. 22.7%), and so not clinically significant.
Image: CC/Wiki
©2016 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.