#VisualAbstract: Oxygenated hypothermic perfusion reduces post-kidney transplant complications
1. Oxygenated hypothermic machine perfusion (HMPO2) of kidneys donated after circulatory death was associated with fewer severe complications and lower rates of graft failure compared to hypothermic machine perfusion without oxygenation (HMP).
2. There was no significant difference in mean eGFR between HMPO2 and HMP despite potential beneficial effects suggested by analysis of secondary outcomes.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Kidney transplant is the preferred treatment for end-stage renal disease and significantly improves quality of life and survival compared to dialysis. Hypothermic preservation is a cornerstone in reducing ischemic-reperfusion injury and is accomplished clinically through either static cold storage or hypothermic machine perfusion (HMP). However, despite oxygenated HMP (HMPO2) showing promise in animal models, there were no well-designed studies assessing the effect of HMPO2 in kidney transplantation in humans. This randomized, double-blind, paired phase 3 trial comparing HMP with or without oxygenation in kidney transplantations included 106 kidney pairs from donors aged 50 or older after circulatory death. Kidney pairs were transplanted into different recipients with one kidney assigned to HMPO2 and the other to HMP without oxygenation. Results suggested that HMPO2 was safe in kidneys donated after circulatory death and mean estimated glomerular filtration rate (eGFR) was similar at 12 months post-transplant between the HMPO2 and the HMP group. However, significantly fewer severe complications (grade IIIb or greater) and lower graft failure rates were observed with HMPO2 compared with HMP. Notable limitations of the current study include the inability to identify the effect of HMPO2 on acute rejection due to not collecting the necessary data. Additionally, the choice to report eGFR only in pairs of donated kidneys with both kidneys functioning at the 12-month endpoint resulted in the exclusion of informative dropouts which may have been associated with the intervention. Nonetheless, this landmark study is the first to identify that HMPO2 may confer a clinical benefit and has the potential markedly impact clinical practice.
Click to read the study in The Lancet
Relevant Reading: Hypothermic Oxygenated New Machine Perfusion System in Liver and Kidney Transplantation of Extended Criteria Donors: First Italian Clinical Trial
In-Depth [randomized controlled trial]: This randomized, double-blind, paired, phase 3 trial was conducted at 19 transplant centers across Europe and included kidney pairs procured by controlled donation after circulatory death from donors aged ≥ 50 years. A computer-generated randomization scheme was utilized to randomly assign one kidney from each donor pair to HMPO2 and the other to standard HMP without oxygenation. The primary endpoint was estimated eGFR as a marker of renal function at 12 months post kidney transplantation. Between March 15, 2015, and April 11, 2017, a total of 197 kidney pairs were randomized with 106 available for sensitivity and secondary analysis and 83 kidney pairs available for primary outcome analysis.
At 12 months post-transplant, there was no significant difference in mean eGFR in the HMPO2 group (50.5 mL/min per 1.73m2; standard deviation [SD] 19.3) compared to the HMP group (46.7 mL/min per 1.73m2; SD 17.1) with a mean difference of 3.7 mL/min per 1.73m2 (95% CI -1.0 to 8.4; p=0.12). Graft failure at 12-months post-transplant was significantly lower in the HMPO2 group (three (3%) of 106) compared to the HMP group (11 (10%) of 106, hazard ratio (HR) 0.27, 95% CI 0.07 to 0.95; p=0.028). There was no significant difference in patient survival between the HMPO2 group and HMP group (7% vs 8%, HR 0.88, 95% CI 0.32 to 2.41; p=0.80). Fewer severe complications (Clavien-Dindo grade ≥IIIb) were reported in the HMPO2 group versus the HMP group (11%, 95% CI 8% to 14% vs 16%, 95% CI 13% to 20%; p=0.032).
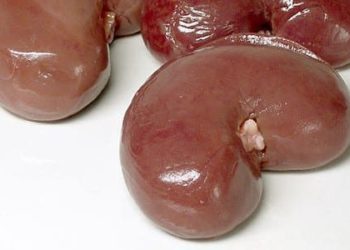
Image: PD
©2020 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.


![Engineered stem cells mitigate liver damage caused by radiation [PreClinical]](https://www.2minutemedicine.com/wp-content/uploads/2014/12/Human_embryonic_stem_cells-350x250.png)