2 Minute Medicine Rewind May 13, 2019
Amyotrophic Lateral Sclerosis versus Multifocal Motor Neuropathy: Utility of MR Neurography
Both multifocal motor neuropathy (MMN) and amyotrophic lateral sclerosis (ALS) affect the peripheral nervous system and present with palsies. Differentiating between these two diseases is important from a prognostic perspective, as MMN should be treated as early as possible with immunomodulatory therapy, while ALS is not currently treatable. Magnetic resonance (MR) neurography has been proposed as a way of differentiating between MMN and ALS. In this cohort study, investigators used MR neurography in 22 participants with ALS, 8 participants with MMN, and 15 matched healthy control participants. The images produced were then given to two blinded readers to examine whether any features of MR neurography could be used to differentiate ALS from MMN and controls. MR neurography images were acquired at mid-thigh, proximal calf, and mid-upper arm of the more clinically affected side. The readers independently rated fascicular nerve lesions and signs of possible denervation using 5-point scales. Investigators found that the mean nerve lesion score was higher in MMN than in ALS (reader 1, score of 2.6 vs. 0.9, p=0.04; reader 2, 3.5 vs. 1.5, p=0.008). Muscle edema and atrophy were found in nearly all participants with ALS and the mean muscle denervation score was significantly higher in ALS than in MMN (reader 1, 1.82 vs. 0.25, p=0.002; reader 2, 2.59 vs. 1.13, p=0.007). Mean muscle denervation score was also higher in ALS than healthy controls (p<0.001 for both readers). There were no differences in signs of muscle denervation between participants with MMN and healthy controls (p=0.99 and p=0.73 for the two readers). The inter-rater agreement between the two readers was kw =0.73 (95% CI 0.59 to 0.87) for nerve lesions and kw=0.61 (95% CI 0.44 to 0.77) for muscle denervation signs. The sensitivity for detection of ALS compared to non-ALS (MMN and control) was 86% (95% CI 67% to 95%), and the specificity was 100% 95% CI 86% to 100%). The sensitivity of detecting MMN versus non-MMN (ALS and control) was 88% (95% CI 53% to 99%), and the specificity was 100% (95% CI 91% to 100%). The results from this study suggest that MR neurography can be used as a way of differentiating MMN with ALS, with signs of nerve denervation playing an important role. This study was limited by its small size and the heterogeneity of treatment and disease duration amongst participants.
Human prion disease, also known as Creutzfeldt-Jakob disease (CJD), is a neurodegenerative disease caused by abnormally folded prion proteins. The progression of CJD is rapid, with time from diagnosis to death being approximately 4 to 6 months. Currently, there is a need to more accurately predict disease duration in order to improve clinical management and stratify patients for clinical trials. Fluid biomarkers have been studied as a way to predict disease course in sporadic CJD (sCJD). In this cohort study, investigators performed neurological tests and collected cerebral spinal fluid (CSF) and blood from 188 participants with sCJD in order to examine the association between fluid biomarkers and disease progression. Investigators found that greater baseline levels of total tau (t-tau) were associated with shorter survival; this was true for both plasma (HR 5.8, 5% CI 2.3 to 14.8, p<0.001) and CSF (HR 1.6, 95% CI 1.2 to 2.1, p<0.001). Plasma and CSF t-tau levels were correlated (r=0.74, 95% CI 0.50 to 0.90 p<0.001). Plasma neurofilament light (NfL) levels, CSF nFL levels, total tau: phosphorylated tau ratios, and neuro-specific enolase levels were other fluid biomarkers associated with survival. Codon 129 genotypes of the PNRP gene and Barthel index were also associated with survival time. The results from this study suggest that using plasma and CSF t-tau levels could contribute important predictive information for patients with sCJD. It is important to note, however, that this study was limited with only a relatively small subsample of patients with all plasma and CSF biomarkers.
Efficacy of Adjunctive Infliximab vs Placebo in the Treatment of Adults With Bipolar I/II Depression
Depressive symptoms are an important part of bipolar disorder types I/II and contribute to significant morbidity and mortality. Establishing treatments for bipolar disorder has been difficult; in fact, no existing treatments approved by the FDA have been developed using an a priori disease model, and multiple failed clinical trials have suggested multiple biotypes within the heterogeneous population of bipolar disorders. In a previous clinical trial, infliximab, a tumor necrosis factor antagonist, was not found to have a significant effect over placebo in adults with major depressive disorder and bipolar disorder. Post-hoc analysis, however, suggested that infliximab could have an effect in patients with immune-inflammatory activation. In this randomized controlled study, investigators randomized 60 patients with bipolar disorder who met 1 biochemical or phenotypic inflammatory criteria at baseline to receive infliximab or placebo in order to study the effect of infliximab on patients with bipolar disorder and some evidence immuno-inflammatory activation. Participants were required to meet 1 of the following biochemical or phenotypic inflammatory criteria at baseline: CRP of 5 mg/L or more; obesity, and increased triglyceride levels, decreased high-density lipoprotein cholesterol level, or elevated blood pressure; type 1 or 2 diabetes; inflammatory bowel disorder; rheumatologic disorder; daily cigarette smoking; or migraine headaches. Investigators found that at 12 weeks, there were no between-group differences in treatment response (χ2=0.07, p=0.79). There were also no differences in remission rates (χ2=0.004, p=0.95). In a subgroup analysis, investigators also analyzed patients who had experienced physical abuse in childhood, and found that higher levels of physical abuse were associated with higher response rates amongst infliximab-treated patients at week 12 (RR 0.88, 95% CI 0.81 to 0.96, p=0.003). Overall, the results from this study do not support the use of infliximab as a treatment for bipolar disorder when given to patients based on inflammatory criteria. It should be noted, however, that the criteria for inflammation was broad due to a need for recruitment. Infliximab may have a role in treating patients with a history of childhood physical abuse, however, this finding requires further research due to the small sample size evaluated in this study.
Glucagon-containing α-cells are important for regulating glucose homeostasis along with insulin-secreting β-cells. Glucagon receptor antagonists (GRAs) hold potential as antidiabetic therapies, but there is a concern that GRAs may cause α-cells to proliferate. While studies evaluating this have been carried out in rodents, these have been limited to young mice, raising questions surrounding the effect of GRAs in adult mice and adult animals in general. In this controlled study, investigators gave a highly selective GRA (JNJ-46207382) to both young and adult mice in order to examine the effect of GRAs on measured α-cell turnover and proliferation. Investigators found that in young mice, the GRA caused a 2.5 fold greater α-cell proliferation. In adult mice, administration of the GRA also resulted in α-cell proliferation, but this proliferation was 60% less than what was observed in young mice. In both young and adult mice, pancreas mass was unaltered by the GRA studied, and islet histology was also normal. Taken together, the results from this study suggest that administration of GRA causes a greater degree of expansion of α-cells in young mice as compared to older mice. This has implications for potential GRA use in middle-aged or elderly patients who may have minimal α-cell proliferation. This study was limited, however, in that it used a single GRA molecule in a rodent model that may or may not be generalizable to humans. The mice used in this study were also non-diabetic, therefore, the effect of GRAs on diabetic α-cells requires further study.
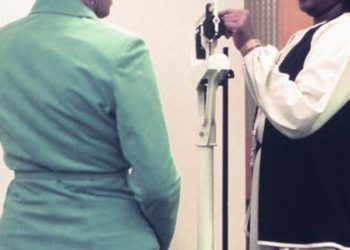
Association of Visual Impairment With Economic Development Among Chinese Schoolchildren
Children in many developing countries have poor vision. In China, poor vision accounts for nearly half of all childhood disability. China has been experiencing unprecedented economic growth over the last several decades, however, this does not necessarily translate into improvement across all domains of health. In this retrospective cohort study, investigators analyzed data from 1,951,084 children in China from 1995 to 2014 in order to examine trends in visual impairment and identify any association with economic factors. The GDP in China increased from $1263 to $7594 over the time period studied. Investigators found that after adjusting for multiple demographic characteristics, every 100% increase in GDP from 1995 to 2014 was associated with a 20% increase in the prevalence ratio of visual impairment (VI) (PR 1.20, 95% CI 1.20 to 1.21). This association between GDP increase and VI was stronger in males (PR 1.22 for males, 95% CI 1.21 to 1.23, vs. PR 1.19, 95% CI 1.18 to 1.19 for female, p<0.001). Rural areas and younger age groups were also increasingly affected during the time period studied. Geographically, more economically developed regions had higher prevalence of VI for all survey years. The results from this study suggest that China’s economic development is associated with the increase in VI in children, which has implications for global health practices and policies as China and other countries continue to develop. This study, however, is limited in that it was cross-sectional nature; the results do not establish a causal relationship.
Image: PD
©2019 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.