Childhood febrile seizure characteristics associated with epilepsy diagnosis [Pediatrics Classics Series]
Image: PD
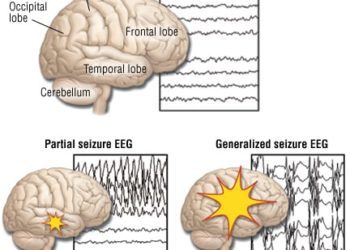
1. Through the inclusion of infants from the Collaborative Perinatal Project, this large, multicenter, prospective study found that children with febrile seizures, complex febrile seizures (seizures that were longer than 15 minutes in duration, occurred more than once in 24 hours, or had focal neurologic findings), and febrile seizures of earlier onset (before 6 months of age) were at increased risk of developing epilepsy when compared to individuals who had febrile seizures without these features.
2. Abnormal performance on neurologic testing was linked to increased epilepsy risk.
Original Date of Publication: November 1976
Study Rundown: With previous research indicating an increase in unprovoked seizures following childhood febrile seizures, researchers in this study were the first to try to define the risk factors associated with progression from childhood febrile seizure to epilepsy. As a part of the Collaborative Perinatal Project of the National Institute of Neurological and Communicative Disorders and Stroke, researchers were able to complete this multi-center, large prospective cohort study. Children were followed from birth to age 7 with febrile and afebrile seizure activity and development noted over the course of the study. Individuals who experienced febrile seizures with and without complex features, those who tested abnormally on developmental screening prior to their first febrile seizure, and children with early febrile seizure presentation were significantly more likely to be diagnosed with epilepsy by the age of 7. This study was limited by its lack of consideration of potential covariates including whether or not a child was started on anticonvulsant therapy. The connection between febrile seizures and future epilepsy is still recognized with further studies confirming the connection although the incidence of epilepsy occurring after a non-complex febrile seizure remains very small.. Other studies have found early first febrile seizures (before 5 years of age), along with repeated febrile seizures, prolonged febrile seizure length, and a family history of cerebral palsy as potential contributors to childhood epilepsy.
Click to read the study in The New England Journal of Medicine
In-Depth [multi-center, prospective cohort study]: From 12 teaching hospitals, 54 000 children born to mothers enrolled in the Collaborative Perinatal Project were recruited for study inclusion. Children were followed from birth to 7 years of age. Parents were interviewed regarding the occurrence of seizures, convulsions, and changes in consciousness at 4, 8, 12, 18, and 24 months with annual follow-up continuing from 2 to 7 years of age. Interviews were completed by trained individuals. Medical records were also obtained for each medically managed seizure episode. Neurologic and developmental assessments were completed throughout the study with standard physical examination at 4 months of age, psychological assessment at 8 months of age, and pediatric and neurologic assessment at 1 year of age. “Febrile seizures” were defined as any seizure along with fever in a child 1 month to 7 years of age. “Afebrile seizures” were defined as recurrent seizure without fever before 4 years of age or 1, isolated afebrile seizure episode after 2 years of age. “Epilepsy” was defined as recurrent afebrile seizures with at least 1 occurring after 2 years of age. No associated known acute neurologic illness could be present in order for these diagnoses to be made. Complex features of seizures were defined as seizure duration longer than 15 minutes, more than 1 seizure in 24 hours, and focal seizure activity.
Of the children included, 1706 experienced at least one febrile seizure and were followed to study completion at 7 years of age. Among these children, 550 (32%) had at least one more febrile seizure, but no afebrile seizure, while 52 children (3%) had at least 1 afebrile seizure during the study and 34 (2%) met criteria for a diagnosis of epilepsy. Of the 39 179 children who did not have a febrile seizure and were followed for 7 years, 199 were diagnosed with epilepsy. Significantly more individuals were diagnosed with epilepsy following a first febrile seizure with complex features when compared to those with only afebrile seizures (41 v. 5 per 1000, X2 = 70, p < 0.001). Children with complex febrile seizures had significantly greater rates of epilepsy than those who had febrile seizures without complex features (41 v. 15 per 1000, X2 = 7.8, p < 0.01). Children with febrile seizures without complex features were diagnosed at higher rates than those who had afebrile seizures (15 v. 5 per 1000, p < 0.001). Children with any abnormal findings on assessments prior to first seizure were significantly more likely to meet criteria for epilepsy when compared to those with normal screenings (39 v. 12 per 1000, X2 = 11, p < 0.001). An 18-fold increase in risk of epilepsy was noted among children who had both complex first febrile seizure and abnormal screening performance compared to those with no febrile seizure (92 v. 5 per 1000, X2 = 79, p < 0.001). Previously normal children without complex seizures had significantly higher rates of epilepsy than those with afebrile seizures (11 v. 5 per 1000, X2 = 4.0, p < 0.05). There was a significant increase in epilepsy by 7 years of age among children who had febrile seizures during their first 6 months of life when compared to those who had them beyond the first year (57 v. 15 per 1000, X2 = 7.6, p < 0.01).
© 2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.