Omecamtiv mecarbil may be associated with decreased risk of heart-failure events
1. Patients who received omecamtiv mecarbil had slightly fewer systolic heart failure exacerbations compared to those who received placebo.
2. Serious adverse events occurred equally frequently in both groups.
Evidence Rating Level: 1 (Excellent)
Study Rundown: At present, no medications that directly stimulate systolic function have been shown to improve health outcomes in patients who have heart failure with a reduced ejection fraction. Several calcitropes have been able to augment measures of cardiac performance, but the increase in the magnitude of intracellular calcium transients was found to also heighten the risk of myocardial ischemia, ventricular arrhythmias, and death. Omecamtiv mecarbil is the first of a class of myotropes called cardiac myosin activators which selectively enhance binding of the head domain to actin filaments, thereby increasing cardiac output without modulating calcium availability. In a phase 2 trial, this medication appeared to be effective in increasing stroke volume and reducing both heart rate and plasma natriuretic peptide levels. Based on these findings, the present phase 3 study was designed to evaluate the effect of omecamtiv mecarbil treatment on the incidence of heart-failure events and cardiovascular death in patients with a reduced ejection. While both groups had similar mortality from cardiovascular causes as well as all causes, the omecamtiv mecarbil group had significantly fewer instances of the composite primary outcome of heart-failure events and cardiovascular death. Further, adverse events generally occurred at similar rates in both groups, although a between-group difference in favor of the omecamtiv mecarbil group was observed with regard to stroke. While this study involved several thousand patients, it was limited by a lack of racial heterogeneity and an underrepresentation of women. Overall, these findings suggested that omecamtiv mecarbil may improve clinical outcomes in patients with systolic heart failure.
Click here to read the study in NEJM
Relevant Reading: Chronic Oral Study of Myosin Activation to Increase Contractility in Heart Failure (COSMIC-HF): a phase 2, pharmacokinetic, randomised, placebo-controlled trial
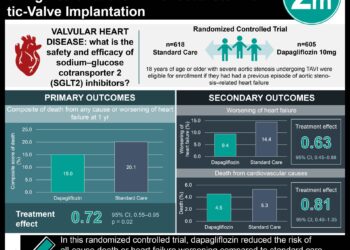
In-Depth [randomized controlled trial]: This double-blind study, termed Global Approach to Lowering Adverse Cardiac Outcomes through Improving Contractility in Heart Failure (GALACTIC-HF), was conducted from January 6, 2017 to August 7, 2020 and involved 8232 individuals between 18 and 85 years of age who had symptomatic heart failure with a left ventricular ejection fraction of 35% or less. Patients were randomly assigned in a 1:1 ratio to receive either placebo or oral omecamtiv mecarbil at a dose of 25 mg, 37.5 mg, or 50 mg twice daily according to the plasma levels of the drug. The primary outcome was a composite of cardiovascular death or a heart-failure event, defined as an urgent clinic visit, emergency department visit, or hospitalization leading to treatment intensification beyond a change in diuretic therapy. This composite outcome occurred in 1523 of 4120 patients (37.0%) in the omecamtiv mecarbil group and in 1607 of 4112 patients (39.1%) in the placebo group (hazard ratio [HR], 0.92; 95% confidence interval [CI], 0.86 to 0.99; P=0.03). The individual outcome of death from cardiovascular causes occurred in 808 patients (19.6%) in the omecamtiv mecarbil group and in 798 patients (19.4%) in the placebo group (HR, 1.01; 95% CI, 0.92 to 1.11; P=0.86). All-cause mortality was also nearly identical between groups (1067 patients vs. 1065 patients; HR, 1.00; 95% CI, 0.92 to 1.09). With regard to safety, both groups had similar numbers of patients for whom treatment was temporarily withheld because of concern of active myocardial infarction or ischemia (103 vs. 101) as well as patients for whom treatment was discontinued due to adverse events (371 vs. 382). The omecamtiv mecarbil group also had a slightly greater increase in median cardiac troponin I and slightly greater decreases from baseline in heart rate and median NT-proBNP; all other laboratory measures were similar between groups.
Image: PD
©2021 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No articleshould be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.