One-year follow-up of patients receiving transcatheter aortic valve replacement reported
1. One year after transcatheter aortic valve replacement (TAVR), the incidence of stroke was 4.1%, overall mortality was 23.7% and 46.8% of patients who were alive had not been rehospitalized.
2. Several baseline characteristics were independently associated with 1-year mortality, including advancing age, severe lung disease, end-stage renal disease, and male sex.
Evidence Rating Level: 2 (Good)
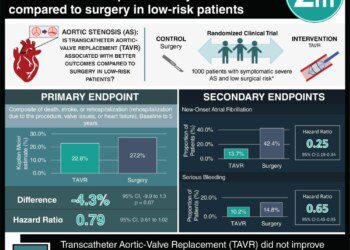
Study Rundown: Transcatheter aortic valve replacement (TAVR) has emerged as a minimally invasive alternative to surgery for patients with severe aortic stenosis who cannot undergo surgery. Given its relatively recent adoption in medical practice, long-term follow-up of patients to assess clinical outcomes has not yet been performed, with a previous study of patients in the Society of Thoracic Surgeons/American College of Cardiology (STS/ACC) Transcatheter Valve Therapies (TVT) Registry reporting outcomes at only 30 days post TAVR.
This study aimed to investigate the rate of stroke, death and re-hospitalization in patients 1 year after receiving TAVR. At 1 year, the rate of stroke was 4.1%, the rate of mortality was 23.7%, and 46.8% of patients alive at the end of the year did not experience readmission. The limitations of this study stem from the dataset used for analysis, which has some shortcomings such as no report of cause of death. There is also no data on outcomes in patients receiving surgical aortic valve replacement; therefore, it is not possible to assess the comparability of the two procedures. Nevertheless, the outcomes of this study provide important information to be presented to patients considering TAVR.
Click to read the study, published today in JAMA
Relevant Reading: Outcomes Following Transcatheter Aortic Valve Replacement in the United States
In-Depth [retrospective cohort]: This study followed a cohort of 12,182 patients from the STS/ACC TVT Registry for patients who had TAVR performed between November 2011 through June 2013. In-hospital death occurred in 5.2% (633 patients) of the cohort, stroke in 1.9% (231 patients) and transient ischemic attack in 0.3% (34 patients). At 30 days, 2.5% of the cohort experienced stroke and 7.0% of the cohort experienced death. At 1 year, the incidence of stroke was 4.1% and mortality was 23.7%. Within the timeframe of the year, 24.4% of patients were hospitalized once, 12.5% were hospitalized twice and 11.6% were hospitalized three or more times. The causes of hospitalization were heart failure, repeat aortic valve intervention and a composite of stroke/heart failure or repeat aortic valve intervention, from most common cause to least common. The following baseline factors were associated with increased mortality at 1 year: increased age, male sex, severe COPD, end-stage renal disease, non-transfemoral access, history of atrial fibrillation/atrial flutter and increased Society of Thoracic Surgeons Predicted Risk of Mortality (STS PROM) score.
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.



![Type I diabetes not associated with early menopause [OVADIA study]](https://www.2minutemedicine.com/wp-content/uploads/2014/12/diabetes1_edited-75x75.jpg)

