Sirolimus may prevent graft failure in patients with renal transplant for antiphospholipid syndrome
1. Antiphospholipid syndrome (APLS) in an autoimmune condition causing mechanical endothelial injury leading to activation of a pathway that triggers vascular stenosis; this pathway is initiated by a kinase referred to as mammalian target of rapamycin (mTOR).
2. Inhibition of the mammalian target of rapamycin (mTOR) with sirolimus was linked to a decreased recurrence of APLS nephropathy and improved graft survival in post-renal transplant patients.
Evidence Rating Level: 2 (Good)
Study Rundown: Antiphospholipid syndrome (APLS) is an autoimmune condition with both primary and secondary etiologies that often results in antibody-mediated vascular thrombosis and obstetrical complications. In addition, patients with APLS also develop vascular cellular infiltrates which is thought to also contribute to the increased incidence of stroke, myocardial infarction, mesenteric ischemia and nephropathy.
Mammalian target of rapamycin (mTOR) is a kinase involved in multiple cell signaling pathways. This study is the first to examine the role of mTOR in APLS and whether blockade of this pathway, as achieved by sirolimus, can be linked to clinically significant vascular stenosis. Among those with APLS nephropathy leading to end-stage renal disease, post-renal transplant recurrence commonly results in allograft failure. For this reason, mTOR inhibitors have been hypothesized to prevent APLS-mediated activation (which would lead to vascular stenosis and subsequent graft failure) in post-renal transplant APLS patients.
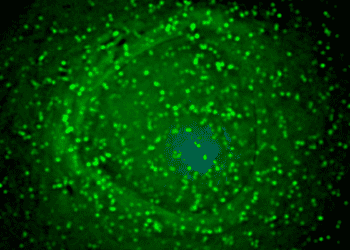
In-vitro cellular studies (extracted from renal vascular sections) were first conducted; this demonstrated that renal vascular endothelial cells from APLS patients had higher levels of a phosphorylated proteins downstream of the mTOR pathway (i.e. S6RP and AKT). To then demonstrate a link between APLS and mTOR activation, antibodies from the serum of APLS were incubated with control endothelial cells which also showed similar levels of phosphorylated proteins. However, this response was successfully suppressed with cells incubated in sirolimus for 48 hours. As observed in-vitro, post-renal transplant patients with APLS who were on sirolimus also had decreased phosphorylation of S6RP and AKT on renal biopsies taken at 3 and 12 months post-op. More importantly, APLS patients transplanted had higher graft survival at a mean follow up of 82 months (70%).
Post-transplant patients for APLS nephropathy were specifically examined in this study, therefore the effects of mTOR inhibition cannot be generalized to preventing all types of vascular stenosis. However, given the pleiotropic effects of mTOR in cellular signalling, it is possible that in the future, inhibition of this pathway may provide a way to prevent vascular stenosis in other organs.
Click to read the study, published today in NEJM
Click to read an accompanying editorial in NEJM
Relevant reading: “Black swan in the kidney”: Renal involvement in the antiphospholipid antibody syndrome
In-Depth [retrospective cohort]: The initial part of this study focused on in-vivo studies using renal vascular cells from patients (both with and without APLS) to confirm the association between APLS and mTOR pathway activation (ie. phosphorylation of downstream proteins S6RP and AKT) as well as sirolimus suppression of mTOR.
Within a large cohort of renal transplant recipients between January 2000 and December 2009, 37 recipients were identified as being positive for antiphospholipid antibody and a matched group of 74 recipients negative for antiphospholipid antibody were included into this study. Recipients in both groups were randomized (based on physician preference) to immunosuppression with either a calcineurin inhibitor or sirolimus. At a mean follow up of 82 months, transplant recipients with antiphospholipid syndrome receiving sirolimus have a graft survival of 70% (7/10) versus 11% (3/27) in those not receiving sirolimus. However, this benefit with sirolimus was not observed for transplant recipients without antiphospholipid antibody.
More from this author: Brodalumab effective in treating active psoriatic arthritis, Idelalisib plus rituximab improves progression-free survival in relapsed CLL, SSRI use during pregnancy not linked to increased risk of autism,Combo antifungal therapy most effective treatment for cryptococcal meningitis
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.




![Paracetamol (Tylenol) ineffective for low-back pain [PACE Study]](https://www.2minutemedicine.com/wp-content/uploads/2014/07/479px-Extra_Strength_Tylenol_and_Tylenol_PM-75x75.jpg)
![Macitentan better than placebo for preventing progression of pulmonary arterial hypertension [SERAPHIN Trial]](https://www.2minutemedicine.com/wp-content/uploads/2013/08/ca68dc0329bef0b42ccae7b6656a0f_gallery-75x75.jpg)