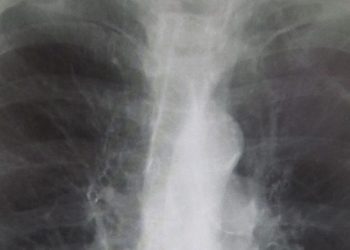
The NETT: Lung-volume-reduction surgery in emphysema
Image: PD
1. Lung-volume-reduction surgery significantly improves exercise capacity, but not overall survival, in patients with emphysema when compared with medical therapy
2. Post hoc subgroup analyses showed that in patients with upper-lobe emphysema and low baseline exercise capacity, lung-volume-reduction surgery significantly decreased mortality compared to medical therapy
Original Date of Publication: May 22, 2003
Study Rundown: While lung-volume-reduction surgery had been proposed as a treatment option for patients with severe emphysema, there was little evidence examining its effects. The National Emphysema Treatment Trial (NETT) was the first study to assess the morbidity, mortality, and therapeutic benefits of lung-volume-reduction surgery for emphysema patients. The findings of the trial showed that the lung-reduction significantly improved patients’ exercise capacity compared to medical therapy, but did not significantly change overall survival (RR 1.01, p=0.90). Post hoc subgroup analyses demonstrated that surgery significantly reduced mortality in patients with upper-lobe emphysema and low exercise capacity (RR 0.47, p=0.005) and significantly increased mortality in patients with non-upper-lobe emphysema and high exercise capacity (RR 2.06, p=0.02) when compared with medical treatment. A major criticism of this trial centres on the survival differences demonstrated in specific subgroups based on post hoc analyses, as opposed to predefined analyses.
In summary, results of this study suggest that lung-volume-reduction surgery can significantly improve exercise capacity in patients with emphysema. While subgroup analyses did demonstrate survival benefits in patients with upper-lobe emphysema and low exercise capacity at baseline, these findings should be interpreted with caution given that they were performed post hoc.
Click to read the study in NEJM
In-Depth [randomized controlled trial]: This was a randomized, controlled trial that enrolled 1,218 patients from 17 clinics from across the United States. The list of inclusion and exclusion criteria is lengthy – generally, patients were eligible if they had clinical and radiological evidence of emphysema, were non-smokers for at least 4 months, completed all pre-rehabilitation assessments, and were considered fit for surgery. Each patient’s distribution of emphysema (i.e., predominantly upper-lobe vs. predominantly non-upper-lobe) was determined by high-resolution CT. The primary outcome measures were overall mortality and maximal exercise capacity as measured by cycle ergometry. The secondary outcome measures included pulmonary function, distance walked within six minutes, and quality of life, as determined by self-administered questionnaires. Prior to randomization, patients underwent 6-10 weeks of supervised pulmonary rehabilitation. Patients were then randomly assigned to receive lung-volume-reduction surgery (i.e., bilateral stapled wedge resection via median sternotomy or video-assisted thoracic surgery) or medical therapy, and then re-evaluated after 6, 12, and 24 months of follow-up. Improved exercise capacity was defined as a 10 W increase in workload during cycle ergometry.
At 90 days, the mortality rate in the surgery group was significantly higher than the medical therapy group (7.9% vs. 1.3%, p<0.001). There was no significant difference in mortality rates when comparing patients who underwent median sternotomy and video-assisted thoracic surgery (8.6% vs. 6.1%, respectively, p=0.33). Total mortality rates were not significantly different between the two groups at a mean follow-up of 29.2 months (RR 1.01, p=0.90). Patients receiving surgery had significantly improved exercise capacity as measured by cycle ergometry at 6 (28% vs. 4%, p<0.001), 12 (22% vs. 5%, p<0.001), and 24 months (15% vs. 3%, p<0.001) than the medical-therapy group. Post hoc subgroup analyses revealed that surgery patients with upper-lobe disease and low-exercise capacity had a lower mortality rate (RR 0.47, p=0.005) and experienced significantly improved exercise capacity (30% vs. 0%, p=0.005) when compared with similar patients receiving medical therapy only. In patients with non-upper-lobe disease and high baseline exercise capacity, mortality was significantly higher in the surgical group (RR 2.06, p=0.02).
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.



![2 Minute Medicine: Pharma Roundup: Price Hikes, Breakthrough Approvals, Legal Showdowns, Biotech Expansion, and Europe’s Pricing Debate [May 12nd, 2025]](https://www.2minutemedicine.com/wp-content/uploads/2025/05/ChatGPT-Image-May-12-2025-at-10_22_23-AM-350x250.png)