#VisualAbstract: Preterm formula is similarly effective to human milk fortifiers as breastmilk supplement
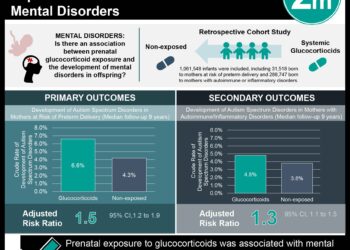
1. Low-weight infants fed with breast milk supplemented with pre-term formula had noninferior weight gain compared to infants fed with breast milk supplemented with commercial human milk fortifiers (HMF).
2. The incidence of feed intolerance was lower in low-weight infants fed with breast milk supplemented with pre-term formula compared to infants fed with breast milk supplemented with HMF.
Evidence Rating Level: 1 (Excellent)
For low-birth weight infants, human milk does not provide adequate nutrients at usual feeding volumes. Therefore, several human milk fortifiers (HMF) have been developed as breast milk supplements to supply high nutrient requirements of low-birth weight infants. However, HMFs do pose potential risk of complications such as feed intolerance and necrotizing enterocolitis (NEC) and are very costly, which may preclude accessibility in low-and-middle income countries.
This new noninferiority randomized trial was conducted to determine if preterm formula (PTF) was as clinically effective as HMF supplementation. 123 low-birth weight infants receiving at least 100 ml/kg/d of feeds and consuming 75% of milk or more were randomized to breast milk fortified with PTF (60 participants) or HMF (63 participants). Neonates with major congenital abnormalities were excluded. The primary outcome was rate of in-hospital weight gain from randomization. Overall, there was no difference in weight gain observed between groups up to time of discharge or at 40 weeks’ corrected gestational age. Furthermore, infants in the PFT group had lower incidence of complications such as feed intolerance and NECs. Lastly, the cost differential for PTF was around $0.3 per day, which was significantly lower than that of HMF (around $4 per day). Overall, these findings demonstrated that PFT was a non-inferior, safe, and lower-cost fortification strategy that may be more widely accessible and used. However, a study with longer post-discharge follow-up and a systematic cost-effectiveness analysis would be needed to better understand the clinical efficacy and feasibility of implementing this measure globally.
Click to read the study in JAMA Pediatrics
Image: PD
©2021 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.