Lopinavir-ritonavir not associated with clinical benefit in patients with severe COVID-19
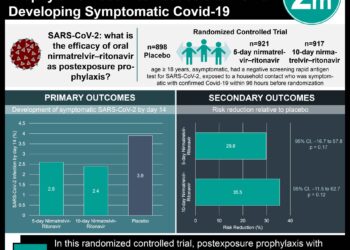
1. In this randomized controlled trial involving adults hospitalized with confirmed SARS-CoV-2 infection, treatment with lopinavir-ritonavir in addition to standard supportive care did not yield appreciable benefit.
2. No significant difference between groups was observed in mortality, viral RNA loads, or duration of detectability.
Evidence Rating Level: 2 (Good)
Study Rundown: The novel coronavirus SARS-Cov-2 is known to cause the respiratory illness Covid-19 in varying degrees of severity, but no therapeutic agents have been demonstrated to be effective in combating coronavirus infections. Lopinavir is an HIV type 1 aspartate protease inhibitor that has shown in vitro activity against both SARS and MERS, but the concomitant use of other drugs, the lack of randomization, and the dependence on historical control groups in previous trials has precluded analysis of its efficacy and safety. This open-label trial involving hospitalized adults with laboratory-confirmed COVID-19 found no significant difference in the time to clinical improvement between the lopinavir-ritonavir and standard-care groups. In addition, mortality and the percentage of patients with detectable viral RNA at various time points were similar between groups. While serious adverse events were less common in the lopinavir-ritonavir group, gastrointestinal adverse events occurred more frequently. Limitations of this study were that a significant percentage of patients in the treatment group were unable to complete the full course of administration and that the overall mortality was nearly twice as high as initially reported by descriptive studies. These findings limit the generalizability of the study’s results as it is possible that a less severely ill population may reap greater benefits from the trial regimen. Future studies involving more heterogeneous populations or different combinations of antiviral agents will continue to guide strategy in addressing this new pandemic.
Click here to read the study in NEJM
Relevant Reading: A systematic review of lopinavir therapy for SARS coronavirus and MERS coronavirus—A possible reference for coronavirus disease‐19 treatment option
In-Depth [randomized controlled trial]: 199 adults hospitalized with Covid-19 in Wuhan, China were individually randomized in a 1:1 ratio to receive either lopinavir-ritonavir (400 mg and 100 mg, orally) plus standard care or standard care alone, defined as supplemental oxygen, noninvasive and invasive ventilation, antibiotics, vasopressor support, renal-replacement therapy, and extracorporeal membrane oxygenation as needed. Placebos were not prepared due to the trial’s emergent nature. In the intention-to-treat population, no significant difference in time to clinical improvement was detected between groups (median, 16 days vs. 16 days; hazard ratio for clinical improvement, 1.31; 95% confidence interval [CI], 0.95 to 1.85; P=0.09). In the modified intention-to-treat population, there was a small but significant difference in time to clinical improvement (median, 15 days vs. 16 days; hazard ratio, 1.39; 95% CI, 1.00 to 1.91). The time to clinical deterioration was also similar between groups (hazard ratio for clinical deterioration, 1.01; 95% CI, 0.76 to 1.34). These findings were independent of the timing of initiation of treatment (either within 12 days of the onset of symptoms or later). While duration of hospitalization did not vary between groups, lopinavir-ritonavir patients had a shorter stay in the ICU (median, 6 days vs. 11 days; difference, −5 days; 95% CI, −9 to 0). Finally, while low-grade gastrointestinal adverse events were more common in the treatment group, serious adverse events occurred less frequently (20% vs 32%).
Image: PD
©2020 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.