Metabolic–bariatric surgery associated with reduced all-cause mortality compared to non-surgical management of obesity
1. Matched cohort meta-analysis showed significant morality and life expectancy benefits with metabolic–bariatric surgery compared to non-surgical management of obesity.
2. Survival benefits of bariatric surgery more apparent for individuals with type 2 diabetes.
Evidence Rating Level: 1 (Excellent)
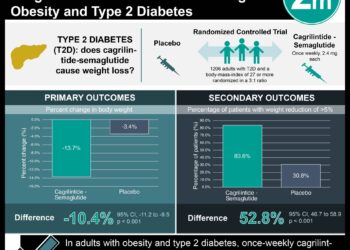
Study Rundown: Metabolic syndrome has been associated with significant morbidity and mortality, increasing rates of cardiovascular disease, certain cancers, and type 2 diabetes. Metabolic-bariatric surgery has been employed as a weight-loss strategy to improve complications associated with metabolic syndrome, but previous studies have not been able to assess efficacy of these surgeries long-term. This one-stage meta-analysis of matched cohort and prospective controlled studies sought to provide a comprehensive assessment of survival benefits after metabolic-bariatric surgery. The results of this study demonstrate that cumulative mortality in patients managed with non-surgical techniques was higher compared to those who underwent metabolic-bariatric surgery. Subgroup analysis of Roux-en-Y gastric bypass, banding, and sleeve gastrectomy all demonstrated this mortality benefit. Median life expectancy was prolonged in the surgical management group. Subgroup analysis showed the number needed to treat to prevent one additional death over 10 years was significantly lower in subgroup analysis for patients with type 2 diabetes. The results of this study support the use of metabolic-bariatric surgery for the management of obesity, particularly in individuals with comorbid type 2 diabetes.
Click to read the study in the Lancet
Relevant Reading: Bariatric surgery for obesity and metabolic conditions in adults
In-Depth [systematic review and meta-analysis]: This study compiled results from 17 randomised trials, prospective controlled studies, and matched cohort studies for metabolic-bariatric surgery vs. non-surgical management, which accounted for 174,772 individuals and 1.2 million patient years. Survival data was evaluated using the Kaplan-Meier method; shared-frailty and stratified Cox models was used to evaluate all-cause mortality. The primary outcome, hazard rate (HR) of death for metabolic-bariatric surgery vs. non-surgical management, showed a 49.2% reduction (95% CI 46.3–51.9, p<0·0001) in favor of surgical management. The median life expectancy for the surgical group was estimated to be 6.1 years longer than the control group (95% CI 5.2–6.9). The number needed to treat to prevent one additional death over 10 years was 24.4 (95% CI 23.1–26.0) for the aggregated cohort, and 8.4 (95% CI 7.8–9.1) for subgroup analysis of individuals with type 2 diabetes; this finding suggests that treatment effect and benefits of metabolic-bariatric surgery are more apparent for those with comorbid type 2 diabetes. Survival benefits and death during follow-up among Roux-en-Y gastric bypass, banding, and sleeve gastrectomy cohorts were similar (between-subgroup heterogeneity I²=3·4%, p=0·36). The limitations of this study are heterogeneity among control cohorts for all included studies, with evidence of participant clustering at the individual study level. Additionally, this study does not account for other pharmacologic and therapeutic interventions patients were receiving. Despite these limitations, this study compiles and synthesizes findings in the field of metabolic-bariatric surgery, compelling demonstrating the survival benefits these procedures confer in the management of obesity, particularly when associated with type 2 diabetes.
Image: PD
©2021 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.