Wellness Check: Sleep
Sound and light interventions improve sleep in critically ill patients
1. In this systematic review and meta-analysis, it was found that among critically ill patients in the intensive care unit, the combination of earplugs, eye masks, and music was the most effective for improving sleep quality.
2. Individually, the most to least effective interventions for better sleep quality were the following: eye masks, bedtime music, quiet time, and earplugs.
Evidence Rating Level: 1 (Excellent)
Sleep quality in the intensive care unit (ICU) is often poor due to high levels of noise and nighttime light. Poor sleep can cause delayed recovery, delirium, and sleep fragmentation for up to a year after discharge in patients with critical illness. While medications for better sleep are available, they have undesirable side effects and may increase the risk of delirium in vulnerable patients. Previous systematic reviews have found that non-pharmaceutical interventions such as earplugs, eye masks, quiet time, and music therapy can be effective in improving sleep quality in ICU patients. The purpose of the present study was to determine the most effective sound and light interventions for improving sleep quality in the ICU.
Of 967 identified records, 24 (n=1507 patients) randomized controlled trials were included from a variety of sources from database inception to August 2021. Studies were included if they evaluated at least one non-pharmaceutical sleep intervention in an adult critical care population and assessed subjective sleep quality as an outcome variable. Studies were excluded if they assessed the efficacy of drug interventions. This meta-analysis was conducted according to PRISMA guidelines and used the Cochrane risk-of-bias tool as well as the Confidence in Network Meta-Analysis application to evaluate risk of bias. A random-effects standard network meta-analysis was performed to determine the effects of sleep interventions. The primary outcome was sleep quality.
The results indicated that a combination of earplugs, eye masks, and music was the most effective intervention for improving sleep quality in the ICU population. When used alone, eye masks were the most effective intervention, followed by bedtime music, quiet time, and earplugs, which had the lowest effect. However, it should be noted that the study only included conscious patients, and therefore the findings may not be generalizable to all ICU populations. Nonetheless, the study highlighted the clinical implications of sound and darkness interventions, which are accessible, non-invasive, and cost-effective methods to improve sleep quality in the ICU.
1. In this randomized controlled trial, the combination of an eye mask sleep position device and oral appliance therapy was significantly more effective than either treatment alone for improving apnea-hypopnea index (AHI) in positional obstructive sleep apnea (OSA).
2. The combination therapy was also associated with higher rates of effective treatment at 6 months compared to either intervention alone.
Evidence Rating Level: 1 (Excellent)
Obstructive sleep apnea (OSA) is a sleep-breathing disorder linked to serious cardiac complications, public safety risks, and higher all-cause mortality. While continuous positive airway pressure (CPAP) is the first-line treatment for OSA, compliance is often poor. A new sleep position therapy device (SPT) featuring an eye mask and blood oxygen monitor, as well as oral appliance therapy (OAT), offer alternative therapies, particularly for those whose OSA is linked to their sleeping position. Therefore, the purpose of the present study was to assess the effectiveness of the combination of SPT and OAT versus either device alone in treating positional OSA.
This randomized controlled trial was conducted at a sleep center in China between May 2019 and December 2020. Out of 312 patients screened, 60 individuals were randomly assigned to the SPT, OAT, or combined intervention groups (n=20 per group). Participants were included if they were between the ages of 18 and 80 years old and exhibited at least one of the following: snored more than 5 days a week with complaints of daytime sleepiness, had at least two other signs or symptoms of OSA, or had a diagnosis of positional OSA with an apnea-hypopnea index (AHI) of over 5 events per hour. Exclusion criteria included severe health conditions that would prevent participation, various dental conditions, latex allergies, and pregnancy. Participants underwent follow-ups at 1 and 6 months following the start of treatment. The primary outcome was a decline in AHI after 6 months. Secondary outcomes included changes in oxygen-derived parameters and curative effect at 6 months, measured by polysomnography.
The results showed that the combined use of SPT and OAT was significantly more effective than either device alone in reducing AHI. The combination therapy was also associated with the highest rates of effective treatment at 6 months. A limitation of the study was that it was conducted in a single center with a small sample size and a low representation of women, limiting its generalizability. Nonetheless, the randomized controlled trial suggested that the combined use of both SPT and OAT offered additional benefits to either treatment alone in treating OSA.
Smartphone usage time is linearly associated with poor sleep quality
1. In this systematic review and meta-analysis, it was found that smartphone overuse was associated with more than a two-fold increased risk of poor self-reported sleep quality among the general population.
2. Furthermore, dose response analysis showed that as smartphone usage time increases, sleep quality is proportionally worse.
Evidence Rating Level: 1 (Excellent)
Excessive smartphone use has become a common issue in our society and has been linked with poor sleep quality. Smartphone use negatively impacts sleep quality through suppressed melatonin secretion from bright light, electromagnetic field exposure, and smartphone content, such as music and violent media. Although many studies have investigated the link between smartphone usage and sleep quality, no systematic review to date has synthesized the current literature. Therefore, the purpose of the present study was to comprehensively analyze the association between smartphone usage time and self-reported sleep quality.
Of 703 records identified from databases between 2010 to 2022, 17 observational studies (n = 36,485 participants) were included. Studies were included if they assessed smartphone overuse and its impact on sleep quality in the general population. Studies were excluded if there was a lack of data, or if they were not published in English. The present systematic review was conducted according to PRISMA guidelines and assessed risk of bias using the Newcastle-Ottawa scale. Restricted cubic spline analysis was used for dose-response analysis. The primary outcome was the impact of smartphone usage on sleep quality.
The results showed that smartphone overuse was associated with more than a two-fold increased risk of poor self-reported sleep quality among individuals, who were mostly students. The dose-response analysis demonstrated that as hours of smartphone use increases, the self-reported sleep quality worsens proportionally. A limitation of the study was that potential confounders such as sex, body mass index, and socioeconomic status were not statistically adjusted for. Nonetheless, the systematic review underlined the impact of smartphone usage on negatively impacting sleep quality.
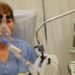
Image: PD
©2023 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.