Māori and Pacific New Zealanders may be disproportionately affected by type 2 diabetes-related clinical outcomes
1. Compared to patients of European descent, poorer health outcomes were seen among Māori and Pacific New Zealanders with type 2 diabetes.
2. Māori patients had the highest incidence rate of all-cause mortality, cardiovascular mortality, and cancer mortality.
Evidence Rating Level: 2 (Good)
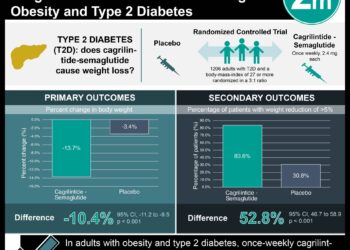
Study Rundown: Disparities associated with ethnicity and socioeconomic status exist in the diagnosis and treatment of diabetes. This retrospective, population-based, longitudinal cohort study compared the rates of mortality and hospital admission between indigenous (Māori), non-European (Pacific), and European patients with type 2 diabetes in Auckland, New Zealand between 1994 and 2018. The primary outcome was to compare the all-cause mortality rate, cardiovascular mortality rate, and cancer mortality rate, as well as the incidence rate of hospitalization due to cardiovascular disease, cancer, and end-stage renal disease (ESRD) between all three ethnic groups. Māori and Pacific patients showed consistently higher hospitalization rates than European patients. Findings were similar with respect to mortality rates with Māori patients reporting a substantially higher incidence of all-cause, cardiovascular, and cancer mortality rates than European patients. This study was limited by heterogeneity in the European, Māori, and Pacific populations with accidental inclusion of patients with type 1 diabetes, as suggested by a high incidence rate of ESRD hospital admissions among patients < 40 years. Nonetheless, this is the first multi-ethnic cohort study to report clinical outcomes of patients with type 2 diabetes in New Zealand over a 24-year period.
Click to read the study in The Lancet Global Health
Relevant Reading: Changing ethnic inequalities in mortality in New Zealand over 30 years: linked cohort studies with 68.9 million person-years of follow-up
In-depth [retrospective cohort]: Between January 1, 1994, and July 31, 2018, 45 072 patients were enrolled in the DCSS (37.2% European, 15.7% Māori, and 26.7% Pacific). Inclusion criteria for this study included patients aged 35-84 years and those with clinically confirmed type 2 diabetes. Patients with type 1 diabetes, prediabetes, gestational diabetes, and those belonging to other ethnic groups were excluded. Enrolled patients were categorized into groups by ethnicity (European, Māori, and Pacific); age (35-44 years, 45-54 years, 55-64 years, 65-74 years, and 75-84 years); sex; and socioeconomic status and were followed until death or the end of the study (July 31, 2018). 21 936 (48.7%) patients were female and the mean age was 56.7 years (SD 13.8). The median follow-up period was 9.7 years (IQR 5.8-13.6). Compared to Māori and Pacific patients, European patients had fewer smokers; lower BMI, HbA1C, and diastolic blood pressure; and less insulin therapy requirement.
Over 24 years, the all-cause mortality rate among patients decreased from 12.62 deaths per 1000 person-years (95% CI 11.05-14.37) in 1994-1998 to 9.90 deaths per 1000 person-years (95% CI 9.14-10.71) in 2014-2018. Compared to European patients, the adjusted incidence rate ratio (IRR) for all-cause mortality was higher in Māori patients (adjusted IRR 1.96, 95% CI 1.80-2.14). Compared to European patients, Māori patients also had higher cardiovascular mortality rates (adjusted IRR 1.93, 95% CI 1.63-2.29) and cancer mortality rates (adjusted IRR 1.64, 95% CI 1.40-1.93). In terms of cardiovascular hospital admission, Māori (adjusted IRR 1.26, 95% CI 1.25-1.28) and Pacific (adjusted IRR 1.09, 95% CI 1.07-1.10) patients with type 2 diabetes were more likely to be hospitalized than European patients. Similarly, when compared to European patients, Māori patients had the highest incidence rate (IRR 2.05, 95% CI 1.96-2.14) of hospital admission due to ESRD, followed by Pacific patients (IRR 1.59, 95% CI 1.52-1.67). Moreover, an increasing trend in incidence rate was observed for cardiovascular, cancer, and ESRD hospital admissions throughout the study period. Findings from this study suggest that indigenous (Māori) and non-European (Pacific) patients have worse clinical outcomes than European New Zealanders who are diagnosed with type 2 diabetes.
Image: PD
©2021 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.