The SOLVD trial: Enalapril in heart failure with reduced ejection fraction [Classics Series]
Image: PD
1. Enalapril significantly reduced the risk of all-cause mortality in patients with congestive heart failure and reduced left ventricular ejection fraction (LVEF≤35%) compared to placebo
2. Patients being treated with enalapril had significantly higher risk of developing elevated serum potassium levels and serum creatinine levels
Original Date of Publication: August 1, 1991
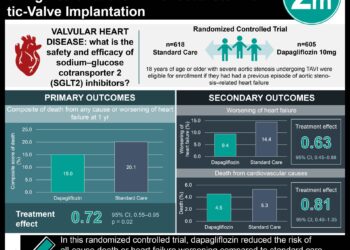
Study Rundown: At the time of the SOLVD trial, some evidence existed to support that angiotensin-converting-enzyme inhibitors (ACE-I) improved hemodynamic stability and reduced mortality in congestive heart failure (CHF) patients. One such study was the CONSENSUS trial, which was published several years before the SOLVD. The CONSENSUS trial, however, only included patients with New York Heart Association (NYHA) Class IV CHF. Given the results of prior studies, the SOLVD trial hypothesized that treatment with an ACE-I would be beneficial to all patients with CHF with reduced ejection fraction, regardless of their NYHA classification. In summary, the SOLVD trial demonstrated that treatment with enalapril significantly reduced mortality (35.2% vs. 39.7%; p<0.0036) and the frequency of hospitalizations for heart failure (25.8% vs. 36.6%; p<0.001) in patients with CHF when compared with placebo.
Prior to enrollment in the trial, there was a run-in period where participants received enalapril for several days followed by approximately two weeks of placebo. This was used as a tool to identify patients who would not tolerate the experimental drug and to assess compliance. This method, however, potentially underestimates the risks of treatment by screening out patients that may have poorly tolerated the drug. It also weakens the external validity of the trial by narrowing the study population of the trial. Nevertheless, the study demonstrated that ACE-I treatment was significant beneficial for patients with all NYHA classes of CHF with reduced ejection fraction.
Click to read the study in NEJM
In-Depth [randomized, controlled study]: This multicenter, randomized, placebo-controlled study, conducted at 83 different hospitals in 3 different countries, randomized 2,569 patients with left ventricular ejection fraction (LVEF) ≤35% to receive either enalapril or placebo. Patients were excluded if they were already taking an ACE-I as part of their CHF management, if they were >80 years of age, or if they were hemodynamically unstable or had severe co-morbidities, such as unstable angina, recent MI, severe pulmonary disease, or severe chronic kidney disease. A run-in period prior to enrollment in the trial included 2-7 days of enalapril 2.5 mg twice daily to assess for adverse reactions and noncompliance, followed by a 14-17 day placebo phase. Doses of enalapril for the treatment group varied from 2.5-10 mg twice daily and were based on the patient’s tolerance of the drug by the participating physician. If a patient’s heart failure worsened over the course of the study, the patient was switched over to open-label treatment. Patients were followed for an average of 41 months. The study outcomes included all-cause mortality, specific causes of mortality, hospitalizations for heart failure, and all hospitalizations.
The mortality rate in the treatment group was significantly lower than that of the placebo group (35.2% vs. 39.7%; p<0.0036). The patients in the enalapril group also had a significant decrease in deaths due to progressive heart failure or arrhythmia (16.3% vs. 19.5%; p<0.0045). Post-hoc sub-group analyses showed that enalapril was beneficial in all 4 NYHA classes of CHF. Not surprisingly, the enalapril group had higher incidence of elevated serum potassium levels (6.4% vs. 2.5%, p<0.01) and creatinine levels (10.7% vs. 7.7%, p<0.01) than the placebo group.
© 2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.